As you may know, there are many varying forms of arthritis.
Sometimes, it is even hard for doctors to figure out which one you may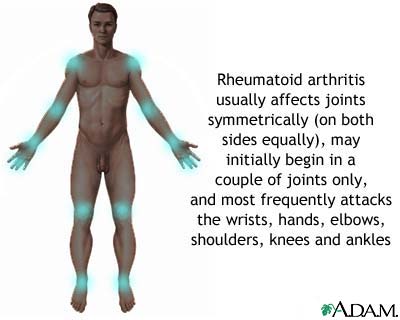 have!
have!
Is it Osteoarthritis or Rheumatoid Arthritis? Lupus? Sjogren’s Syndrome? Ankylosing Spondylitis? Fibromyalgia?
The American College of Rheumatology has a set of guidelines that doctors/rheumatologists are to follow when making an arthritis diagnosis — but, as a patient, you should be made aware, too.
So, how IS Rheumatoid Arthritis diagnosed?
Keep in mind that there is not one, single, specific test just for diagnosing rheumatoid arthritis.
Instead, rheumatoid arthritis is diagnosed based on a combination of: the presentation of the joints involved, characteristic joint stiffness in the morning, the presence of blood rheumatoid factor and citrulline antibody, as well as findings of rheumatoid nodules and radiographic changes such as through X-ray testing and MRIs.
You must communicate your symptoms with your doctor, because at your appointment, your joints may not appear swollen/inflamed, and you might not be in a flare or have any “visible” symptoms. This is where it is important to describe your pain and symptoms in detail. Keeping a health journal or using the Arthritis Track + React online program can help you get your thoughts organized by being able to rely on a list of written symptoms, triggers, flares, and so on.
Once you verbally express your symptoms and concerns with your rheumatologist, they will likely want to order blood work. These labs will test things like the SED Rate, look for inflammation and signs of autoimmunity, and also check out blood tests that can be indicators of RA such as the RA-factor test and certain antibody testing.
The doctor will also probably want to examine how your joints look via x-ray or MRI. They will periodically conduct these imaging tests to compare and contrast changes in the joint.
Doctors may rely on the ACR-EULAR classification criteria for rheumatoid arthritis. This set of guidelines is to help the rheumatologist classify your disease as RA, or not. This document reads as follows:
Target population (Who should be tested?): Patients who
|
|
| Classification criteria for RA (score-based algorithm: add score of categories A–D; a score of ≥6/10 is needed for classification of a patient as having definite RA)‡ |
|
| A. Joint involvement § | |
| 1 large joint¶ | 0 |
| 2-10 large joints | 1 |
| 1-3 small joints (with or without involvement of large joints)# | 2 |
| 4-10 small joints (with or without involvement of large joints) | 3 |
| >10 joints (at least 1 small joint)** | 5 |
| B. Serology (at least 1 test result is needed for classification)†† | |
| Negative RF and negative ACPA | 0 |
| Low-positive RF or low-positive ACPA | 2 |
| High-positive RF or high-positive ACPA | 3 |
| C. Acute-phase reactants (at least 1 test result is needed for classification)‡‡ | |
| Normal CRP and normal ESR | 0 |
| Abnormal CRP or abnormal ESR | 1 |
| D. Duration of symptoms§§ | |
| <6 weeks | 0 |
| ≥6 weeks | 1 |
“The criteria are aimed at classification of newly presenting patients. In addition, patients with erosive disease typical of rheumatoid arthritis (RA) with a history compatible with prior fulfillment of the 2010 criteria should be classified as having RA. Patients with longstanding disease, including those whose disease is inactive (with or without treatment) who, based on retrospectively available data, have previously fulfilled the 2010 criteria should be classified as having RA.
Differential diagnoses vary among patients with different presentations, but may include conditions such as systemic lupus erythematosus, psoriatic arthritis, and gout. If it is unclear about the relevant differential diagnoses to consider, an expert rheumatologist should be consulted.
Although patients with a score of <6/10 are not classifiable as having RA, their status can be reassessed and the criteria might be fulfilled cumulatively over time.”
What it all boils down to is this: diagnosing rheumatoid arthritis and similar diseases can be difficult, even for the best of doctors.
The factors that contribute to difficulty in diagnosis are:
- Patients often find it hard to describe symptoms to doctors in a way that allows them to make the diagnosis.
- Rheumatoid arthritis can appear similar to other common causes of joint pain.
- Patients often think they are feeling “normal” aches and pains and ignore or just live with their symptoms for a long time before seeking treatment. This can lead to irreversible joint damage and worsened conditions.
- Several diseases can masquerade as rheumatoid arthritis and vice versa – a huge part of the problem.
Stay well,
Ashley Boynes
Text the word MOVE to 50555 to give $5 to the Arthritis Foundation!
When prompted please reply with YES to confirm your gift. Msg & Data rates may apply. Full terms at mGive.com/a
“Like” us on Facebook here!
Follow us on Twitter @MidAtlanticAF!

Thanks for posting this. This information really helps people that are suffering on arthritis.